Ladies and gentlemen of the jury, the evidence has been presented. The defendant: elranatamab, a new bispecific antibody treatment for multiple myeloma. The charge: being oversold based on clinical trial data that doesn't quite match the messy reality of actual patients. The verdict? It's complicated.
See, clinical trials are like those perfectly staged home photos on real estate websites—everything's clean, the lighting is flattering, and somehow there's never a pile of laundry on the couch. But when you actually move in, you discover the toilet makes a weird noise and the neighbors have a rooster. This new multicenter study from the U.S. Multiple Myeloma Immunotherapy Consortium is basically the home inspection report for elranatamab.
What Even Is This Drug?
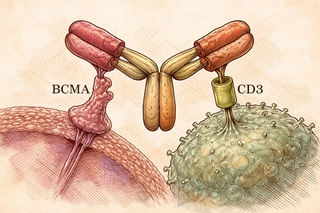
Elranatamab is what scientists call a bispecific antibody. In other words, it's a molecular matchmaker with two arms: one grabs onto BCMA (a protein that myeloma cells love to display like a neon sign), and the other latches onto CD3 on your T-cells. Basically, it drags your immune cells over to the cancer cells and forces an introduction. "T-cell, meet myeloma. Now fight."
The drug earned its stripes in the MagnetisMM-3 trial, which showed impressive response rates in patients with relapsed or refractory multiple myeloma [1]. But here's the thing about clinical trials: they're picky about who gets in. Participants tend to be younger, fitter, and less beaten up by previous treatments than the average patient walking into a cancer center.
The Real-World Report Card
This new study looked at 130 patients across nine U.S. academic centers who received commercial elranatamab [2]. And these weren't your pristine clinical trial candidates. Ninety-one percent were triple-class refractory, meaning they'd already failed three major drug classes. Nearly half were penta-refractory—basically, they'd been through the oncological wringer. Only 22% would have even qualified for the original MagnetisMM-3 trial.
The results? Still pretty good, actually. Sixty-five percent of patients responded, with 36% achieving complete response or better. But—and this is a significant but—the median progression-free survival was 4.3 months, and overall survival was 14.6 months. That's notably shorter than the clinical trial numbers.
In other words, the drug works, just not quite as spectacularly when you're dealing with sicker, more heavily pretreated patients. Shocking absolutely no one who's ever compared a restaurant's Instagram to the actual food that arrives at your table.
The Crystal Ball Problem (Solved?)
One genuinely useful contribution from this study is something called the ALPS score—Anemia-LDH Prognostic System. The researchers found that low hemoglobin and elevated LDH (lactate dehydrogenase, a marker that goes up when cells are damaged) independently predicted worse outcomes.
By combining these two factors, they created a simple scoring system that actually stratifies patients into meaningful risk groups. High ALPS score? Brace yourself. Low score? You've got a better shot. It's the kind of practical tool that could help doctors have more honest conversations with patients about expectations.
The BCMA Problem
Here's where it gets interesting. Nearly half the patients in this study had previously received some form of BCMA-targeted therapy—either CAR-T cells or antibody-drug conjugates. And that prior exposure mattered. Patients treated within one year of their previous BCMA therapy had worse overall survival.
This raises uncomfortable questions about sequencing these treatments. If you've already thrown the BCMA dart once, the target might be a bit harder to hit the second time around. The myeloma cells aren't stupid; they've seen this trick before [3].
The Infection Elephant in the Room
Thirty-eight percent of patients developed infections. That's not a typo. Bispecific antibodies can suppress immune function, and these are already immunocompromised patients we're talking about.
The silver lining? Patients who received intravenous immunoglobulin (IVIG) supplementation had better infection-free survival and even better progression-free survival. Basically, giving patients extra antibodies to replace the ones their dysfunctional immune systems can't make appears to help. The researchers modeled this as a time-dependent covariate, which is statistics-speak for "we tried really hard to make sure this finding is legit."
The Bottom Line
Elranatamab works in the real world—just expect the real-world version, not the airbrushed clinical trial version. For heavily pretreated patients with limited options, a 65% response rate is still meaningful. But the shorter survival times and infection risks mean supportive care isn't optional; it's essential.
The ALPS score gives clinicians a new tool for setting expectations, and the data on IVIG supplementation suggests we might be able to improve outcomes with better supportive strategies. Science rarely delivers clean, simple answers, but it occasionally delivers useful ones.
And that, members of the jury, is a verdict we can work with.
References
-
Lesokhin AM, et al. Elranatamab in relapsed or refractory multiple myeloma: phase 2 MagnetisMM-3 trial results. Nat Med. 2023;29(9):2259-2267. doi:10.1038/s41591-023-02528-9
-
Portuguese AJ, et al. Real-world outcomes with elranatamab in multiple myeloma: a multicenter analysis from the U.S. Multiple Myeloma Immunotherapy Consortium. Blood Cancer J. 2026. doi:10.1038/s41408-026-01477-z
-
Cohen AD, et al. B cell maturation antigen-specific CAR T cells are clinically active in multiple myeloma. J Clin Invest. 2019;129(6):2210-2221. doi:10.1172/JCI126397 PMCID: PMC6546453
-
van de Donk NWCJ, et al. T-cell-redirecting bispecific antibodies in multiple myeloma: current progress and future directions. Blood. 2023;142(11):935-951. doi:10.1182/blood.2022019018
Disclaimer: The image accompanying this article is for illustrative purposes only and does not depict actual experimental results, data, or biological mechanisms.